News
Nutrigenomics Testing — The Cost, Benefits, and ReviewsApr 25, 2024 Stop Guessing, Start Knowing. Choose nutrigenomics testing to provide insights for tailored nutrition and make...
The Origins of Bone Loss: Is Osteoporosis Genetic?Mar 19, 2024 Break free from osteoporosis misconceptions. Explore the power of genetic testing for personalized bone health...

Future of Diabetic Weight Loss Diet is Written in Your DNAMar 15, 2024 Say goodbye to cookie-cutter diets! Explore Genetic Testing for Health for tailored diabetic weight loss...
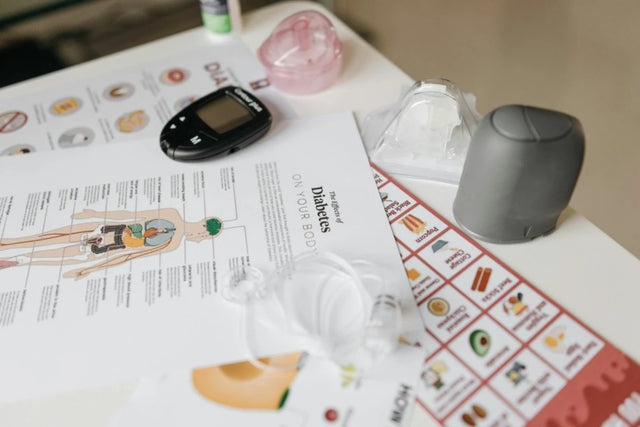
Slimming with Science: Your Guide to 7 Best DNA Tests for Weight ManagementFeb 27, 2024 If you’re struggling to lose weight, you know how frustrating and disheartening it can be....

Beginner's Guide to Oxidative Stress and Antioxidant SupplementsFeb 22, 2024 If you’re reading this, chances are you’ve felt overwhelmed trying to unravel the complex connection...

Oxidative Stress — Your Body's Smoke AlarmJan 30, 2024 Have you ever dragged yourself out of bed, exhausted before your day even started? Or...
The ABCs of DNA Methylation and a Happy, Healthy You!Jan 30, 2024 Have you ever wondered why your health outcomes can differ so much from your siblings...

Is Physical Fitness Genetics?Dec 04, 2023 IS PHYSICAL FITNESS GENETIC? By Annelie Smith. RD IFNCP. Head of Clinical and Mentorship 3X4 Genetics. Physical fitness may mean different things for each one of us. It may involve...


